
DreamerOfDreams
-
Posts
13 -
Joined
-
Last visited
-
Days Won
1
Everything posted by DreamerOfDreams
-
A comment and a question on your regimen:
First, I am a convert! 33 yrs as an episodic sufferer where my cycles are now either every other year or perhaps every year. Went on the regimen last year along with Aimovig (and my usual verapamil) and it seemed to get better, quicker. This year I was noticing the shadows creeping in and jumped back into the regimen and ...knock on all the wood .... shadows are at bay and cycle has not kicked in. While I would love to see a clinical research institute verify your research, I am nonetheless so very thankful for leading the way and helping so many people out.
Second, and apologies if it is covered elsewhere many times but - just had my 25 OH D serum levels tested and I am right at 80 ng/ml. Any advise on how to adjust the regimen to now maintain those levels and not go too high?
thank you!
-
Hey Dreamer,
Thank you for the back-brief. I'm always happy to hear another CHer has found the anti-inflammatory regimen effective in preventing their CH. Your serum 25(OH)D is Spot On at 80 ng/mL. All you need to do is stay on the complete anti-inflammatory regimen at 10,000 IU/day vitamin D3 plus all the cofactors year round!
The normal range of 25(OH)D serum concentrations among 257 CHers responding to this regimen are illustrated in the following normal distribution curve. This data comes from the study that's been running since December of 2011. This is the longest running study of its kind in assessing the effectiveness of vitamin D3 as a CH prophylaxis.
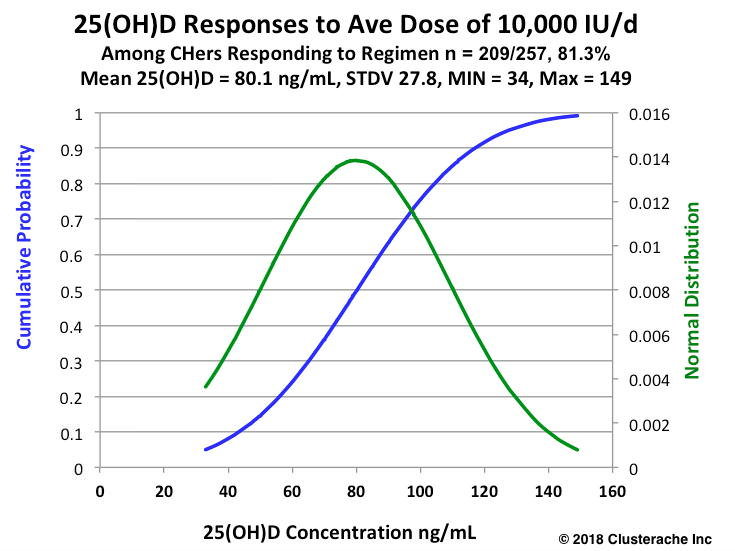
As you can see, the mean 25(OH)D serum concentration among the 209 CHers experiencing a favorable response is 80.1 ng/mL where they experienced an 80% reduction in the frequency of their CH from an average of 3 CH/day down to 3 CH/week in the first 30 days and the 50% of CHers taking this regimen who experienced a complete cessation of all CH symptoms in the first 30 days.
It's best to stay on this regimen year round even if you're an episodic CHer. Your serum 25(OH)D will drop by 14 ng/mL each month you don't take the 10,000 IU/day vitamin D3. As you're episodic and you've stopped taking this regimen after your last cycle, your 25(OH)D serum concentration will have dropped below the pain free threshold when your next cycle comes around. When that happens, the CH beast will jump ugly again... CCHers don't have a choice so take this regimen year round. We call taking this regimen daily a way of life... A very good and healthy way of life at that.
Unless you've already done so, be sure to take the online survey of CHers taking this regimen to prevent their CH. To start this survey, click on the following link:
http://www.esurveyspro.com/Survey.aspx?id=fb8a2415-629f-4ebc-907c-c5ce971022f6
I do have a question for you. Are you still taking the Amovig? As a member of the American Academy of Neurology, I stay abreast of all the anti-CGRP monoclonal antibody (mAb) studies. I've spoken to a molecular biologist about these mAbs and he just laughed... There's no way these mAbs can pass through the blood brain barrier (BBB). Its windows are only 400 Daltons in size, a measure of molecular mass.All of the anti-CGRP mAbs have a molecular mass of 15,000 Daltons so are 37 times too big to pass through the BBB. That means these anti-CGRP mAbs cannot get to neurons within the trigeminal ganglia where CGRP is expressed in the brain and the leading cause of the neurogenic inflammation and pain we know as CH. That also means any therapeutic effect (and it's not all that great) from taking these mAbs is due to a reduction of serum CGRP concentration.
Vitamin D3 has a molecular mass of 385 Daltons and 25-Hydroxy Vitamin D3, a.k.a., 25(OH)D has a molecular mass of 400 Daltons. Accordingly, both pass through the BBB and into neurons within the trigeminal ganglia where they are hydroxylated to 1,25(OH)2D3, the genetically active vitamin D3 metabolite that down-regulates the expression of CGRP to prevent our CH.
So much for your lesson in molecular biology... Thank you again for the update.
Take care and please keep me posted.
Hugs. Peter
-
Batch,
Last cycle I took 3 doses of Aimovig while ramping up on the D3 regimen. Something seemed to work and I had a decent amount of relief until I was off cycle. No way of attributing with certainty the relief to D3, Aimovig, the insanity of the beast or the natural end-of-cycle. This time around I am only using D3...and the cycle seems (fingers crossed) not to be kicking in...but I won't know for sure for a few weeks.
..best to you..
-
Dreamer,
It was the vitamin D3. The dirty little secret Big Pharma doesn't want you to know is the anti-CGRP monoclonal antibodies are too larger to pass through the blood brain barrier so cannot go to the site of action within the nuclei of neurons within the trigeminal ganglia. If the Aimovig provided anything, it was to reduce serum CGRP. Unfortunately that is after the fact as CGRP is experssed from within the sensory neurons creating the pain of CH....
Hugs, Peter
-

